U of M researchers design respirator mask prototypes from filter technology
CSE researchers play key role on the team
MINNEAPOLIS/ST. PAUL (04/06/2020)—The need for N95 masks has skyrocketed in recent weeks in response to COVID-19. To address this challenge, an interdisciplinary research team at the University of Minnesota Twin Cities has designed two respirator mask prototypes from donated filter material by Cummins and bendable components from Bedford Industries.
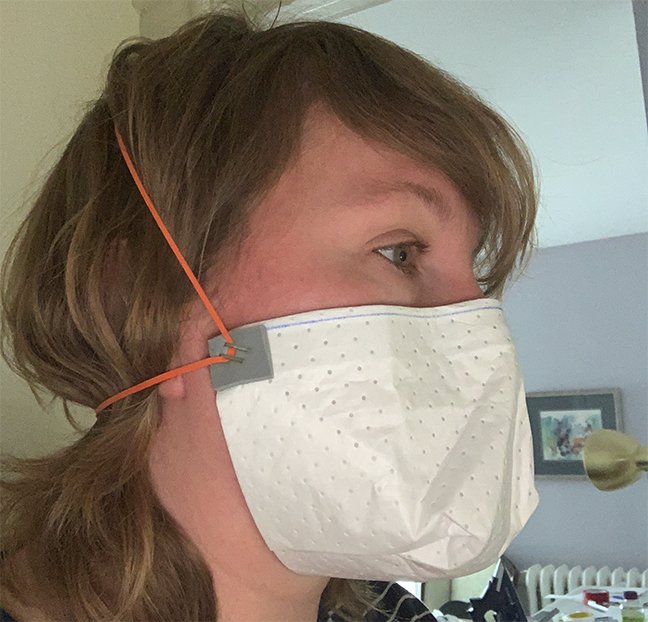
The masks—one modified anesthesia mask and one single-use, disposable mask—are being developed to be close to a N95-equivalent with three distinctive components in mind: ventilation, fit and resilience to supply chain fluctuations. The idea was partly inspired by a process posted on YouTube from the Boston Children’s Hospital.
To accomplish this, researchers had to verify the material would be able to block viruses from being transferred. At the Center for Filtration Research Consortium, David Pui, a mechanical engineering professor in the College of Science and Engineering, and his team were able to test how well the masks would be able to reject virus-containing droplets. His testing results showed that the efficiency of the Cummins material was nearly equivalent to that of filtration material typically found in N95 masks—potentially making the U of M prototypes a viable alternative for health care professionals.

Linsey Griffin, a professor in the College of Design, addressed another key factor in making the masks efficient—sizing and fit. She specializes in understanding the relationship between people’s bodies and highly-functional products, such as personal protective equipment.
“Anytime you are trying to create a product, it is difficult to fit a full population,” Griffin said. “The measurements and proportions of our body are unique to us as individuals, so anytime you make a product for a wide variety of faces, you have to be cognizant of a lot of adjustability features.”
Griffin elaborated that part of the masks’ effectiveness is that the design should eliminate the amount of gaps the particles can pass through by creating a proper seal against the wearer’s face.
“Our goal is to create a product that can be mass produced in a way that doesn’t require the traditional machines and tools that a N95 mask requires,” Griffin said.
Rumi Faizer, an associate professor and chief of the Division of Vascular Surgery in the Medical School, M Health Fairview, highlighted that the research team is using supplies that will not be impacted by potential supply chain shortages. This issue has come into play with filters used in N95 masks.
Faizer, who has also been facilitating clinical setting product testing, noted that donations from Cummins and Bedford Industries has allowed researchers to gain quick access to needed materials.
“Through these international relationships that existed—and the experts that we have in filtration, polymer science, design, engineering and medicine—we were able to quickly build a team to work on new mask designs,” said John Bischof, the research team facilitator and mechanical engineering professor in the College of Science and Engineering who also is the director of the Institute for Engineering in Medicine. “Cummins generously donated many rolls of this filtration material.”
The next steps for the masks is to conceptualize production, which will start with a small group of College of Design students for standardization purposes and adherence to social distancing and quality management. Afterward, the U of M team will look at sterilization and delivery of the masks locally.
“We want physicians, nurses and any health care workers to have the confidence that what they are wearing is going to protect them,” said Griffin.
The U of M team is affiliated with the College of Science and Engineering’s Institute for Engineering in Medicine and Center for Filtration Research Consortium, the Medical School, and the College of Design.
